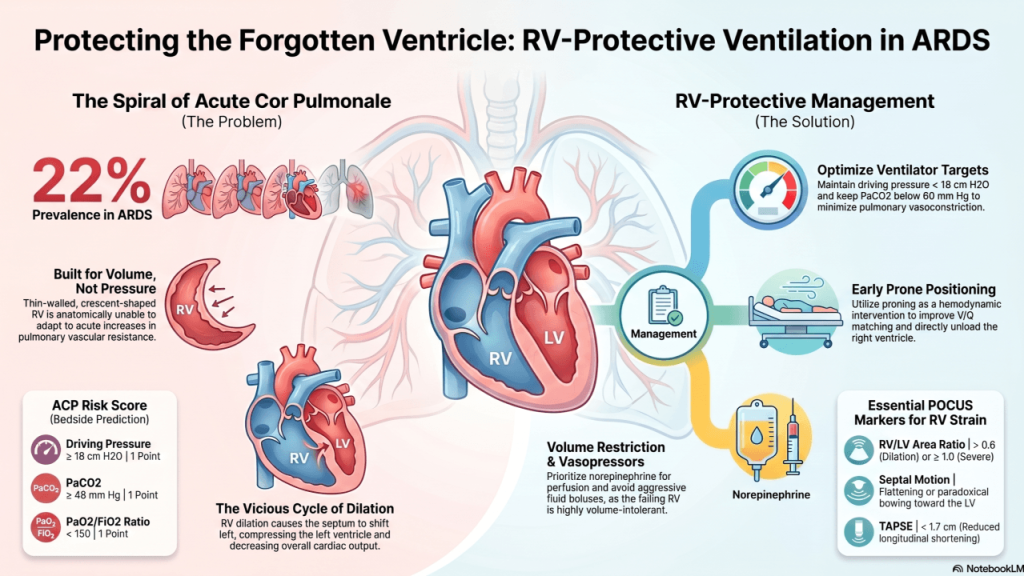
The Forgotten Ventricle Is Killing Your ARDS Patients — and the Ventilator You Are Using to Save Them May Be the Reason Why.
22% of patients with moderate-to-severe ARDS develop acute cor pulmonale on protective ventilation. The right ventricle was never designed to handle pressure — and every PEEP increase, every hypercapnic minute, and every overdistended breath you deliver is loading a chamber that was built to fail. Here is how to recognize it, prevent it, and treat […]