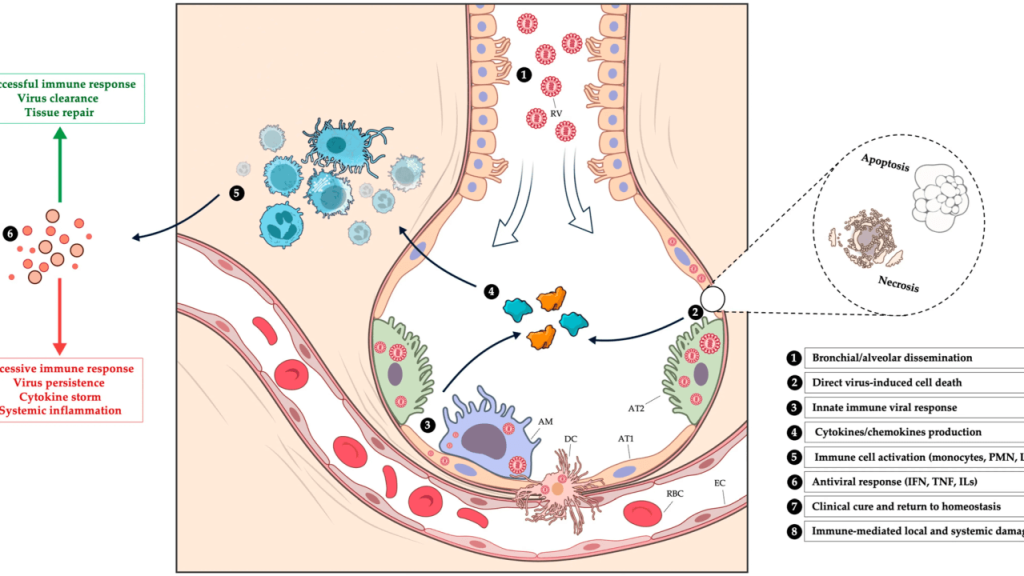
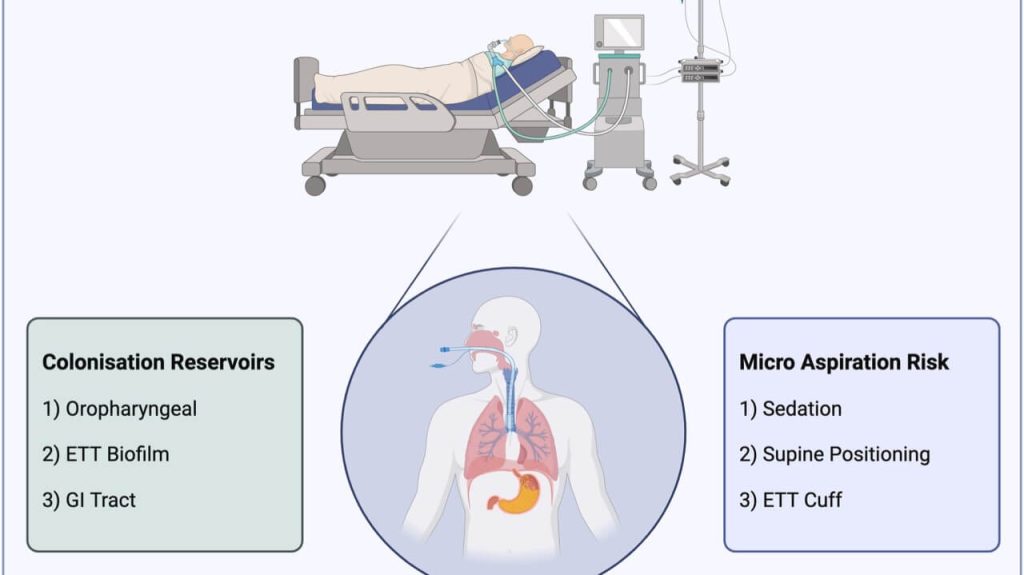
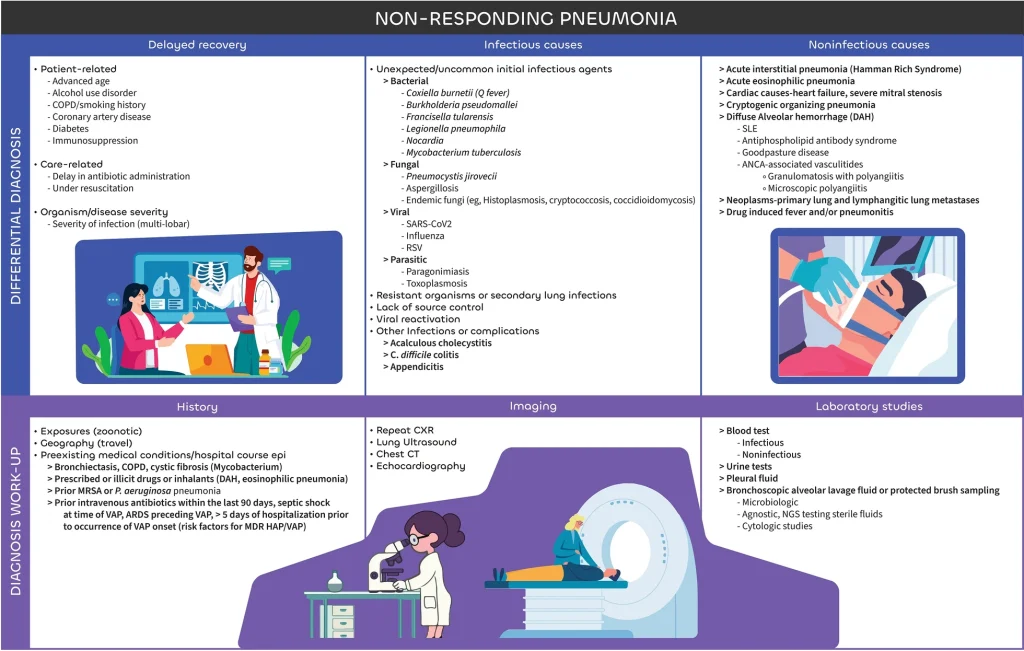
Corticosteroids and hospital-acquired pneumonia
1. Why This Article Matters — Why You Should Read This Corticosteroids are everywhere in critical care. ARDS. Septic shock. COVID-19. Refractory hypoxemia. But when it comes to hospital-acquired pneumonia (HAP) and ventilator-associated pneumonia (VAP), their role remains controversial, inconsistently applied, and poorly understood. This narrative review tackles a clinically uncomfortable reality: While steroids may […]
Corticosteroids and hospital-acquired pneumonia Read Post »