Summary
This commentary explores the clinical utility and challenges associated with critical care continuous electroencephalogram (cEEG) monitoring, particularly focusing on critically ill patients experiencing seizures and status epilepticus. The authors examine recent evidence suggesting limited differences in outcomes between cEEG and routine EEG approaches, highlighting uncertainties around whether seizures observed in critical illness independently contribute to worse outcomes or merely represent an epiphenomenon. Given the significant resource requirements and associated costs of cEEG, the article advocates for careful patient selection and proposes strategies to optimize the allocation of limited EEG monitoring resources based on local availability and clinical scenarios.
Key Points
- Clinical Importance of EEG Monitoring: Continuous EEG monitoring has become increasingly common in ICUs to detect clinically silent seizures, particularly in critically ill patients with acute brain injury or systemic illness, due to limited clinical signs indicating seizure activity.
- Resource Limitations: Despite its clinical appeal, cEEG monitoring remains limited even in well-resourced settings because of high capital equipment costs, staffing demands, and a shortage of EEG-trained professionals, creating barriers to widespread implementation.
- Recent Clinical Trial Outcomes: Two recent randomized controlled trials (RCTs) comparing cEEG monitoring versus intermittent routine EEG showed similar patient outcomes, despite detecting more seizures and providing more aggressive anti-seizure treatments in the cEEG groups, raising questions about the clinical benefit of these interventions.
- Seizures: Harmful or Innocent Bystander?: Although observational studies link higher seizure burdens to worse clinical outcomes, the inability of these studies to fully eliminate confounding factors leaves unresolved whether seizures directly worsen outcomes or merely indicate severe underlying illness.
- Limitations of Current Evidence: Existing RCTs, including those in neonates with hypoxic-ischemic encephalopathy and adults post-cardiac arrest, have yet to conclusively establish a causal link between seizure management via cEEG and improved patient outcomes, mainly due to recruitment challenges and inclusion of severely compromised patients with low survival likelihood.
- Potential Benefit in Select Patient Subgroups: Evidence from subgroup analyses in specific patient populations suggests that certain patients, particularly those experiencing definite EEG seizures without catastrophic brain injury, may benefit significantly from aggressive seizure management guided by cEEG.
- Challenges of Conducting Definitive RCTs: While ideal for answering these clinical questions, large-scale RCTs face significant logistical hurdles such as patient recruitment, consent, timely intervention, and high resource demands, making these studies difficult to conduct.
- Comparative Effectiveness Approach: Given the challenges associated with RCTs, the authors propose comparative effectiveness studies or “natural experiments,” leveraging existing variability in clinical practice to identify patient groups most likely to benefit from cEEG monitoring, although acknowledging potential confounding and resource-related barriers.
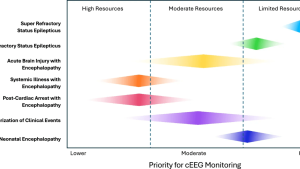
- Proposed Resource-Based Allocation: The article suggests an approach to prioritizing cEEG resources based on center-specific availability:
- Recommendations and Clinical Guidance: Until definitive evidence emerges, clinical decision-making regarding cEEG use should remain flexible and context-specific, guided by patient characteristics, clinical judgment, local preferences, medicolegal considerations, and available resources.
Conclusion
There remains substantial uncertainty regarding the direct clinical benefits of cEEG monitoring and aggressive seizure management in critically ill patients. Clinicians should prioritize careful patient selection and resource allocation, balancing potential benefits against significant costs and logistical constraints. Future robust studies are needed to conclusively determine which critically ill patients derive the greatest benefit from continuous EEG monitoring.

Discussion Questions
- What clinical criteria or biomarkers could reliably identify patients who would benefit most from cEEG monitoring and targeted seizure management?
- How might healthcare systems overcome existing resource limitations to effectively implement cEEG monitoring where it is most needed?
- Given current uncertainties, how can clinicians best communicate the potential benefits and limitations of EEG monitoring to patients’ families and interdisciplinary care teams?
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.