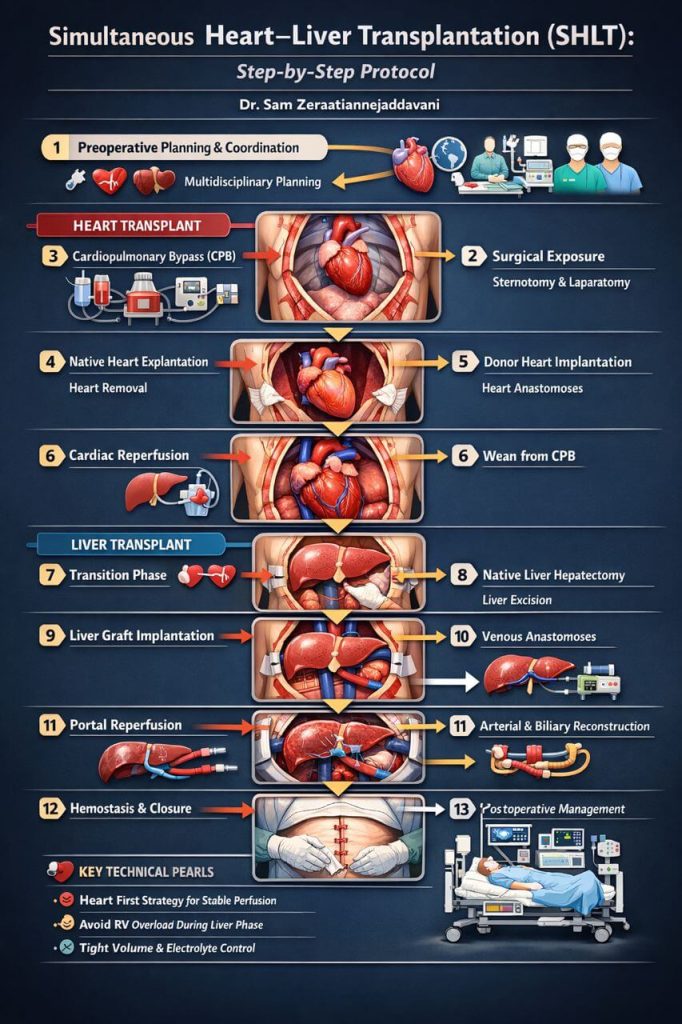
Simultaneos Heart – Liver transplantation
- Home
- Dr. Zeraatian
- Current Page

1. Preoperative Planning & Coordination
•Multidisciplinary alignment (cardiac surgery, transplant hepatology, anesthesia, perfusion)
•Donor organ assessment and synchronized timing of procurement
•Hemodynamic optimization and coagulation planning
•blood products (massive transfusion readiness)
⸻
2. Surgical Exposure
•Median sternotomy + laparotomy (simultaneous or staged)
•Establish invasive monitoring (TEE, PA catheter, arterial lines)
⸻
3. Cardiopulmonary Bypass (CPB) Initiation
•Aortic and bicaval cannulation
•Full CPB support with systemic anticoagulation
•Cooling if required (center-dependent strategy)
⸻
4. Native Heart Explantation
•Transection of great vessels
•Removal of diseased heart while preserving left atrial cuff
⸻
5. Donor Heart Implantation
•Sequential anastomoses (bicaval preferred):
•Left atrium
•IVC → SVC
•Pulmonary artery
•Aorta
⸻
6. Cardiac Reperfusion & Stabilization
•Aortic unclamping and reperfusion
•De-airing and rhythm restoration
•Gradual weaning from CPB
•Critical checkpoint:
•Stable MAP
•Adequate RV function
•inotropes/vasopressors
⸻
7. Transition Phase (Key SHLT Moment)
•Ensure cardiac graft stability before abdominal phase
•Reverse or titrate anticoagulation cautiously
•Optimize volume status to prevent hepatic congestion
⸻
8. Native Liver Hepatectomy
•Mobilization of liver
•hepatic artery, portal vein, bile duct
•IVC management:
•Piggyback (preferred) → preserves venous return
•Standard IVC replacement (if needed)
⸻
9. Liver Graft Implantation
•Venous anastomosis (hepatic veins/IVC)
•Portal vein anastomosis
⸻
10. Portal Reperfusion (High-Risk Phase)
•Controlled reperfusion
•Watch for post-reperfusion syndrome:
•Hypotension
•Hyperkalemia
•Acidosis
⸻
11. Arterial & Biliary Reconstruction
•Hepatic artery anastomosis
•Biliary reconstruction:
•Duct-to-duct (preferred)
•Roux-en-Y (if indicated)
⸻
12. Hemostasis & Closure
•Aggressive correction of coagulopathy
•Drain placement
•Chest and abdomen closure (staged if needed)
⸻
13. Postoperative Management (ICU)
•Integrated cardiac + hepatic support
•RV dysfunction
•Primary graft dysfunction (heart/liver)
•Coagulopathy & bleeding
•Early immunosuppression strategy coordination
⸻
Key Technical Pearls
•Heart-first strategy → ensures stable perfusion for liver graft
•Avoid RV overload during liver phase
•Tight control of volume + electrolytes during reperfusion
•Continuous communication between teams is critical
Dr.Sam Zeraatian Nejad Davani, Cardiovascular and Transplant surgeon. Advanced Fellow of Thoracic Organs Transplantation Chicago Illinois.
We use cookies to provide you with the best possible user experience. By continuing to use our site, you agree to their use. Learn more